Aladent e i patogeni responsabili delle infezioni peri-impianto
in Pubblicazioni recenti
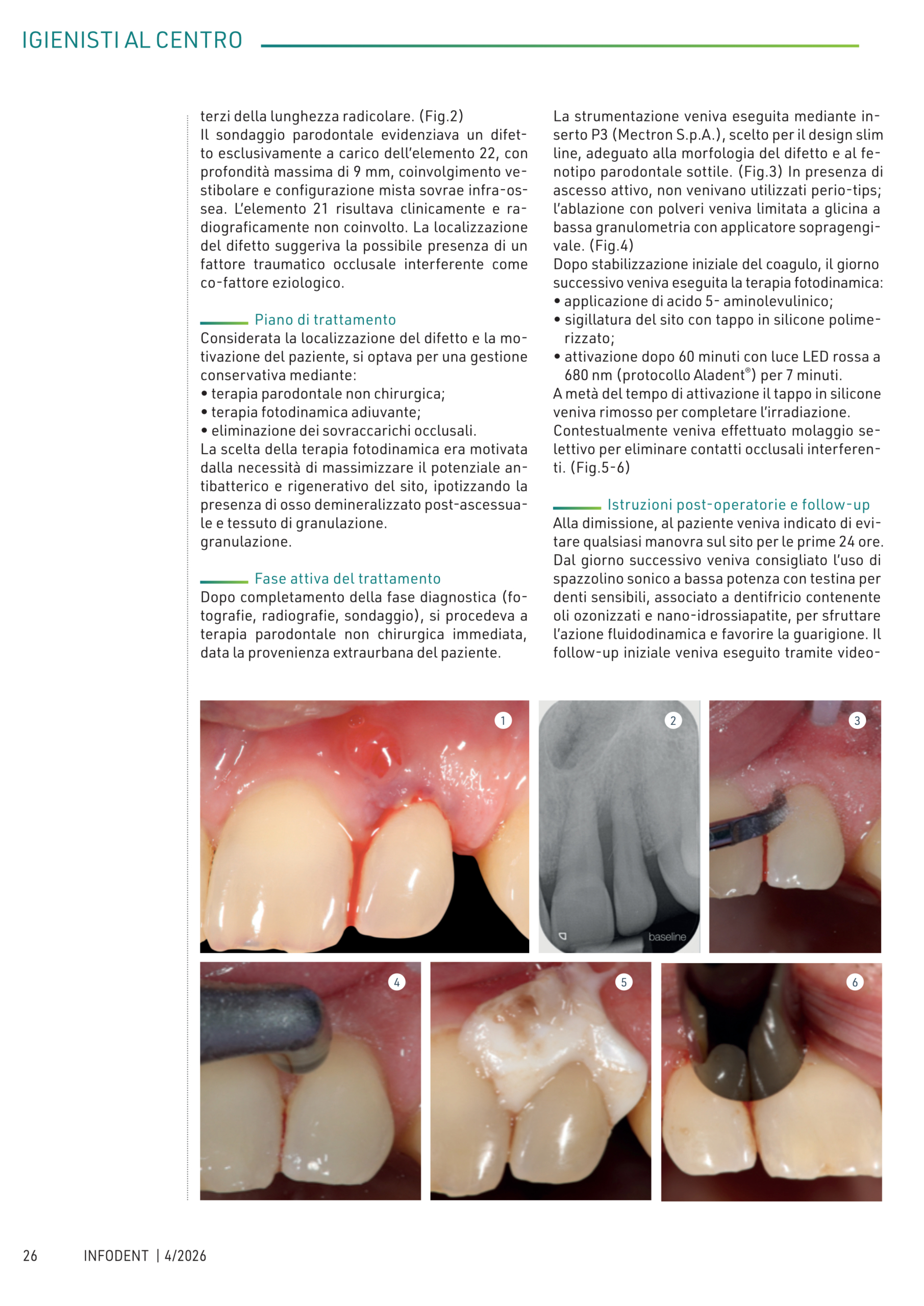
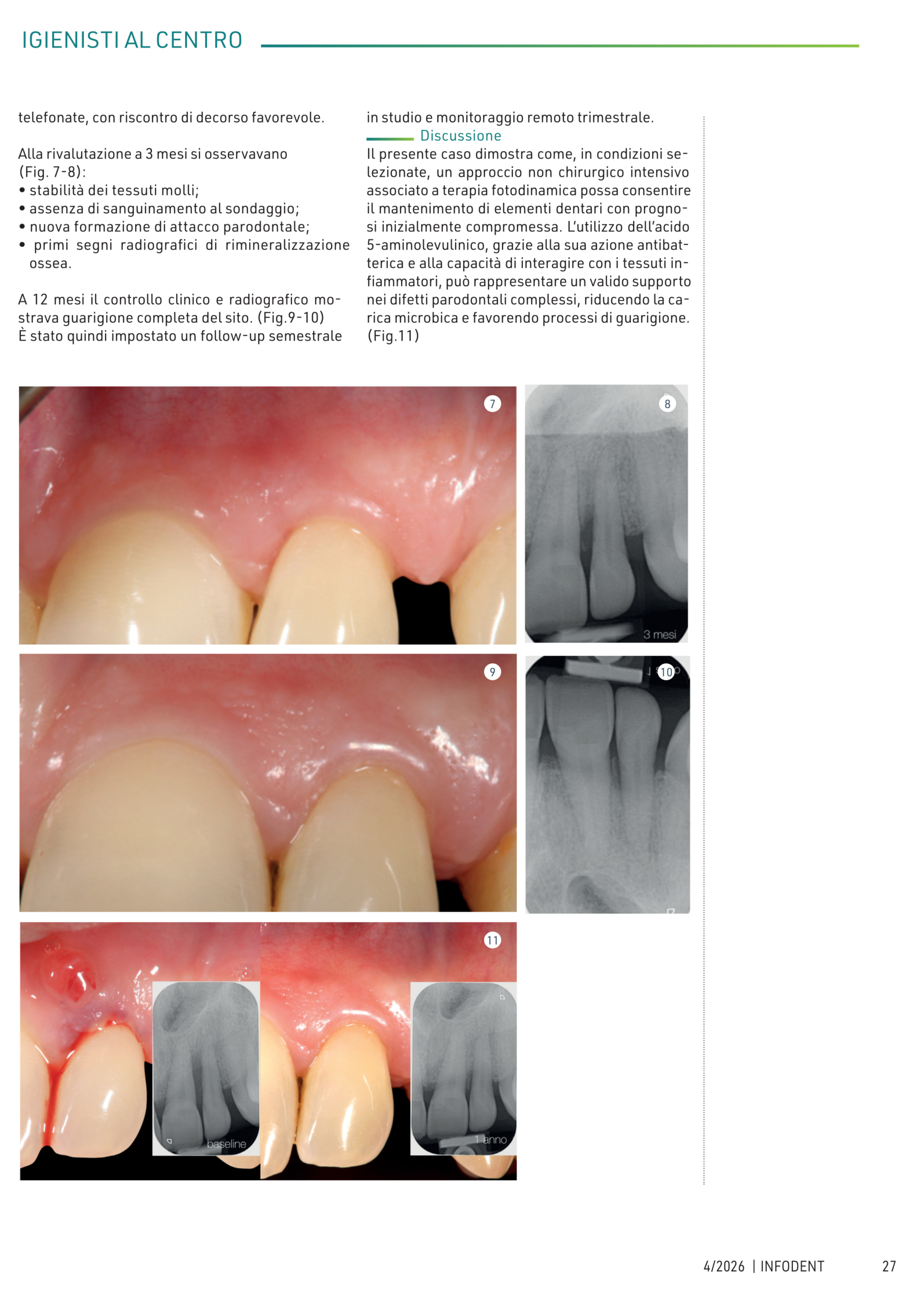
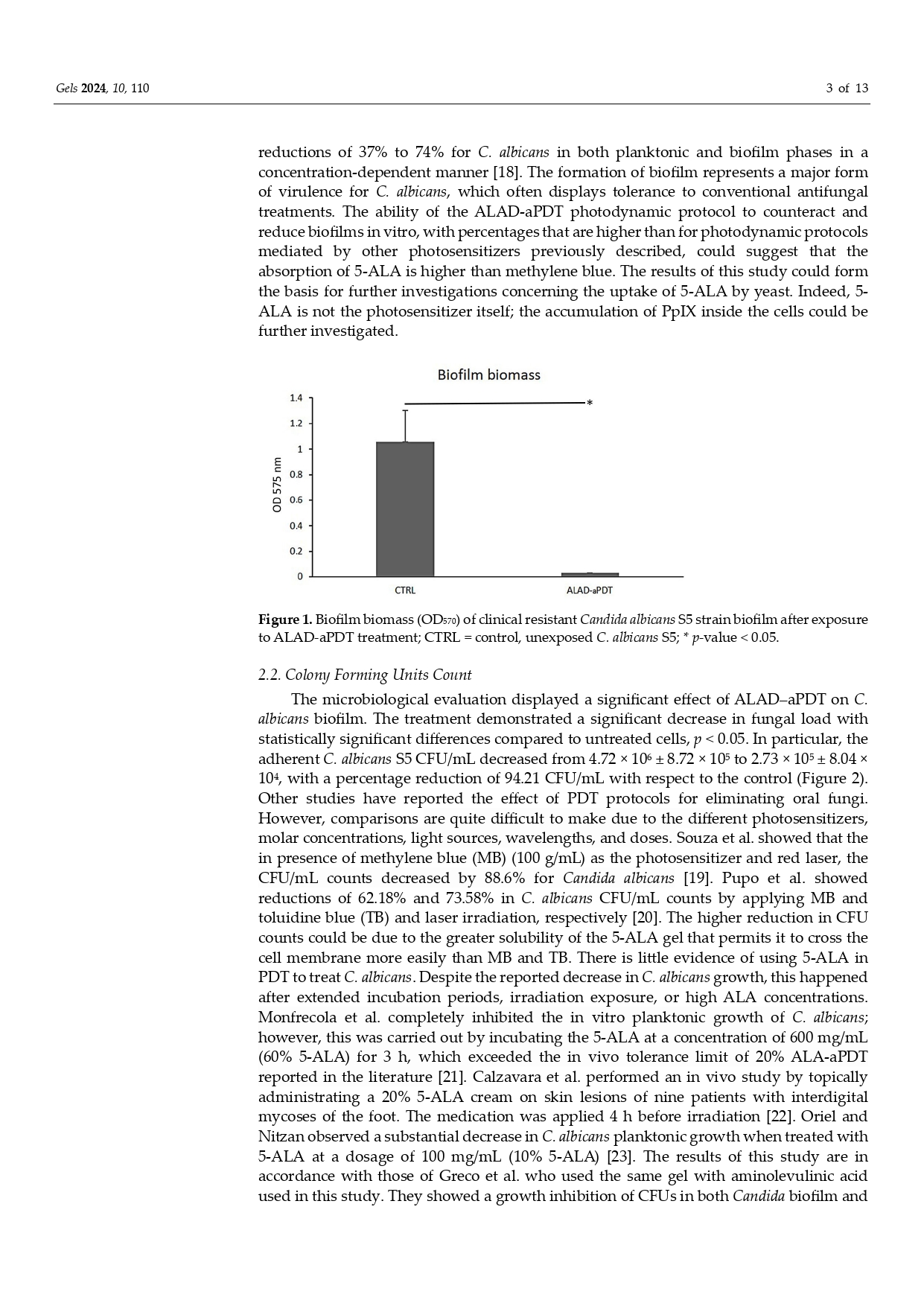
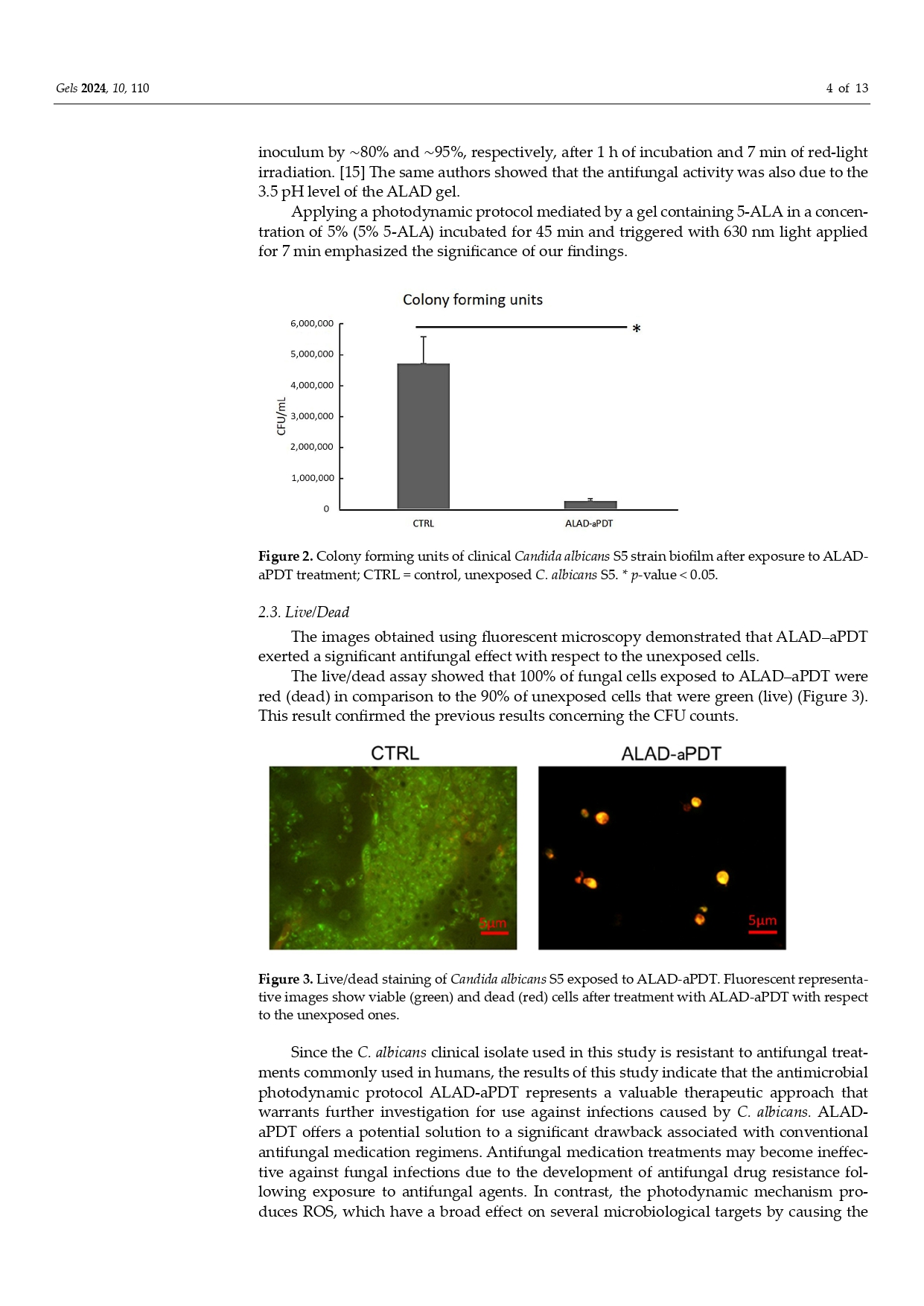
Obiettivo dello studio pubblicato dal prof. Roberto Galvao Dinelli e co-autori, è valutare l’impatto del trattamento Aladent su un modello multispecie di biofilm rappresentativo dei patogeni subgengivali. Il modello scelto è costituito da 33 specie:
- Actinomyces naeslundii
- Actinomyces oris
- Actinomyces gerencseriae
- Actinomyces israelii
- Veillonella parvula
- Actinomyces odontolyticus
- Streptococcus sanguinis
- Streptococcus oralis
- Streptococcus intermedius
- Streptococcus gordonii
- Streptococcus mitis
- Aggregatibacter actinomycetemcomitans
- Capnocytophaga ochracea
- Capnocytophaga gingivalis
- Eikenella corrodens
- Capnocytophaga sputigena
- Campylobacter showae
- Eubacterium nodatum
- Fusobacterium nucleatum vincentii
- Parvimonas micra
- Fusobacterium nucleatum polymorphum
- Fusobacterium periodonticum
- Prevotella intermedia
- Streptococcus constellatus
- Porphyromonas gingivalis
- Tannerella forsythia
- Streptococcus anginosus
- Streptococcus mutans
- Selenomonas noxia
- Propionibacterium acnes
- Gemella morbillorum
- Eubacterium saburreum
- Campylobacter gracilis
Risultati: una sola applicazione di Aladent ha determinato una riduzione significativa ( 70% ) dell’attività metabolica del biofilm oltre a ridurre la popolazione dei batteri, in particolare sulle specie: S. intermedius, V. parvula, A. israelii, P. gingivalis, and E. saburreum.
In conclusione il trattamento con Aladent risulta molto efficace nella riduzione dei biofilm subgengivali, responsabili delle infezioni peri-impianto.
Indagine sull’efficacia antimicrobica e clinica di una nuova tecnologia in endodonzia pediatrica: uno studio in vivo
in Pubblicazioni recentiPubblicato in Applied Sciences giugno 2025
Autori: Luca De Gregoriis, Tatiane Cristina Dotta, Morena Petrini, Silvia Di Lodovico, Loredana D’Ercole, Simonetta D’Ercole, Domenico Tripodi
Abstract:
L’odontoiatria pediatrica è costantemente alla ricerca di trattamenti efficaci e rapidi per i piccoli pazienti, specialmente nell’endodonzia infantile, dove la collaborazione può essere difficile. Questo studio in vivo ha valutato l’efficacia di un nuovo protocollo di terapia fotodinamica (PDT), che utilizza un gel all’acido 5-aminolevulinico (Aladent, ALAD) combinato con luce rossa durante il trattamento canalare dei denti da latte.
Lo studio ha incluso denti decidui che necessitavano di trattamento canalare a causa di carie o traumi, con sintomi clinici di pulpite irreversibile o parodontite apicale acuta. Dopo anestesia locale e isolamento con diga di gomma, le lesioni cariose sono state rimosse e si è proceduto all’apertura della camera pulpare. I canali sono stati preparati con lime manuali, e successivamente è stato applicato il gel ALAD. I pazienti sono stati divisi in due gruppi.
Leggi l’articolo originale
Treatment of a primary superior central incisor after trauma—Group B. (a) Edema present in tooth 61. (b) Preoperative X-ray showing periapical radiolucency. (c) Photoactivation after 1 week placement of the 5-amilovelunic gel inside the root canal. (d) Sample collection using a sterile 0.30. (e) The one-month follow-up radiograph demonstrated bone healing in the periapical area of tooth 61. (f) Clinical examination confirmed the absence of symptoms, with complete resolution of the fistula.
Trattamento non chirurgico della perimplantite. L’impiego di acido5-aminolevulinico a supporto della TNC e il suo ruolo nella biostimolazione tissutale
in Pubblicazioni recentiGli impianti dentali rappresentano una delle opzioni più efficaci per il trattamento dell’edentulia, parziale o totale, consentendo la riabilitazione funzionale ed estetica con un elevato tasso di sopravvivenza a lungo termine. Esistono tuttavia delle controindicazioni alla riabilitazione implantare, così come delle complicanze dovute a fattori individuali, chirurgici o protesici. In particolare, la perimplantite è una delle principali complicanze a lungo termine che può compromettere la durata e la funzionalità di tali dispositivi.
G. Oldoini, S. Pelle, S. Cosola, A. Genovesi
mar. 27 maggio 2025
Articolo pubblicato su Dental Tribune.
Terapia non chirurgica della peri-implantite supportata da tecnologia fotodinamica di seconda generazione
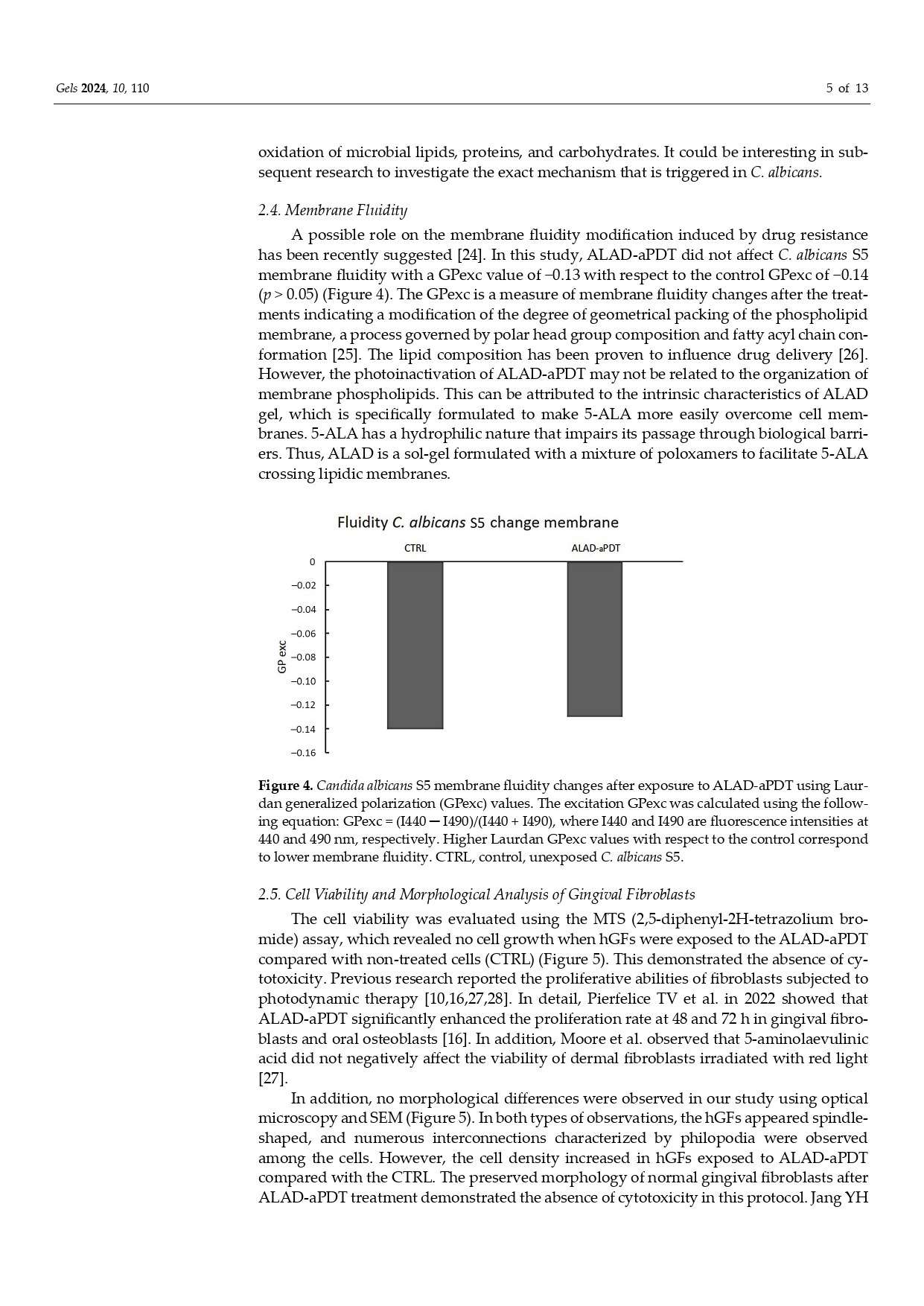
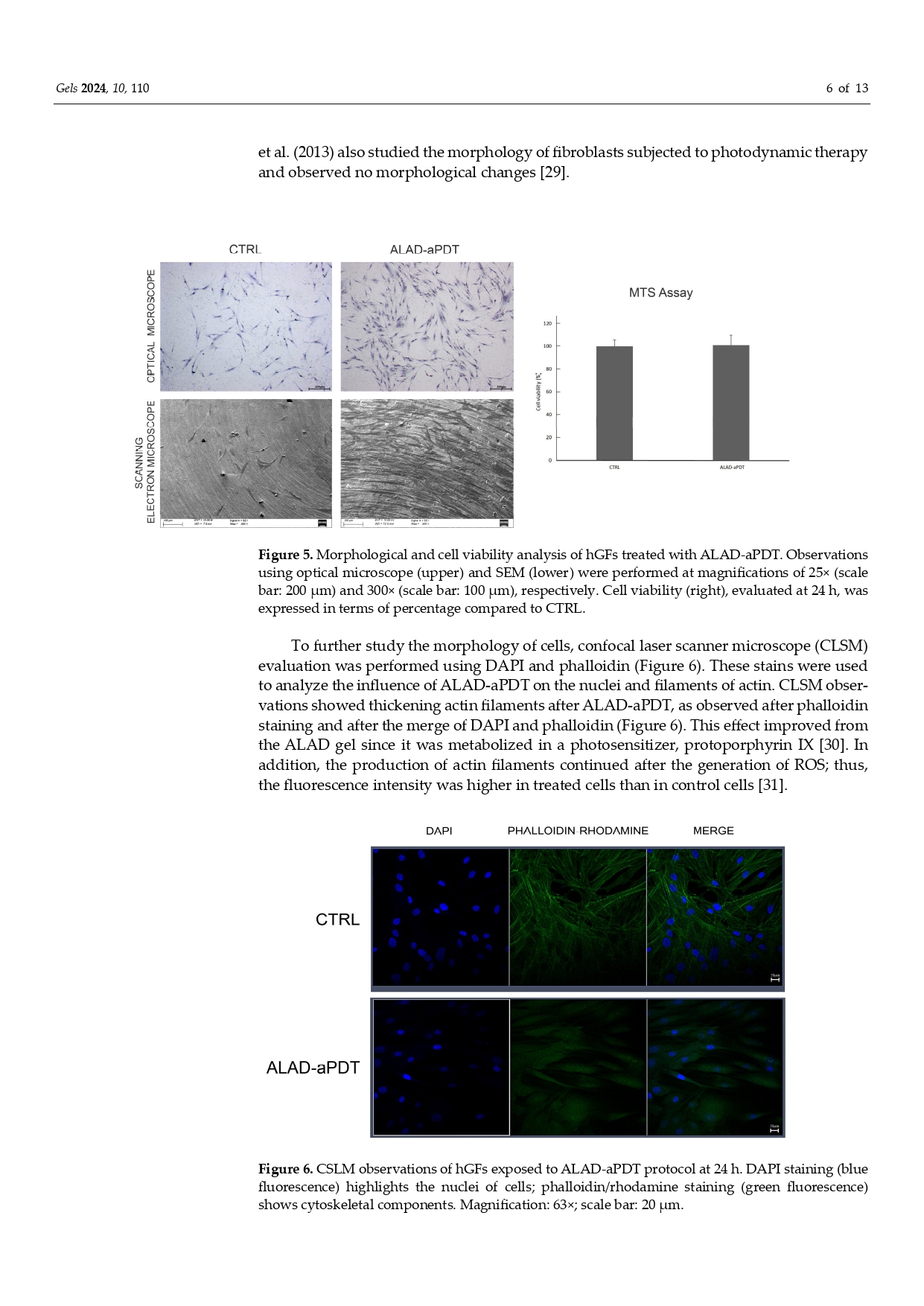
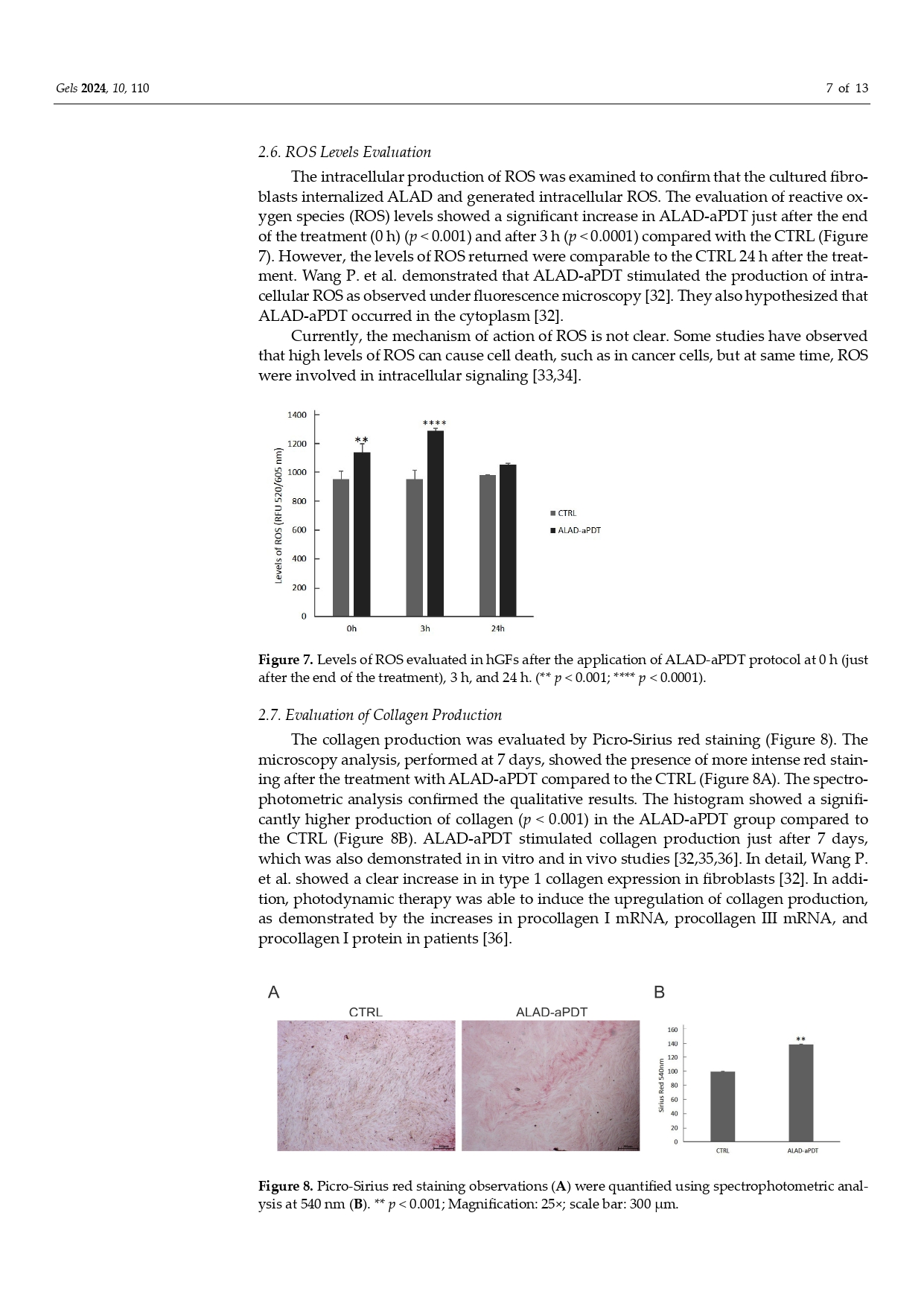
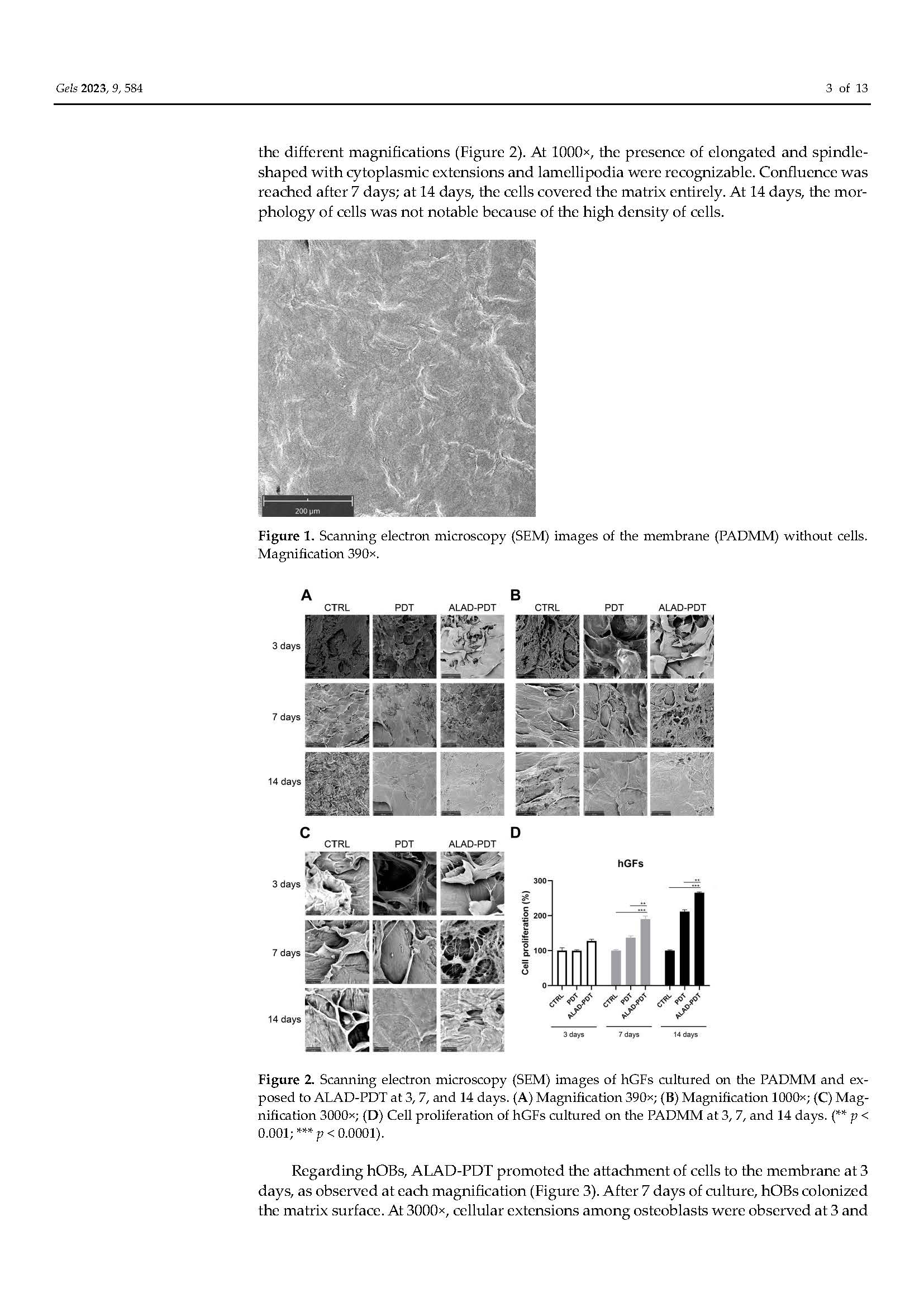
in Pubblicazioni recentiPhotodynamic Therapy with Aminolevulinic Acid Enhances the Cellular Activity of Cells Cultured on Porcine Acellular Dermal Matrix Membranes Used in Periodontology
in Pubblicazioni recentiPhotodynamic Therapy with Aminolevulinic Acid Enhances the Cellular Activity of Cells Cultured on Porcine Acellular Dermal Matrix Membranes Used in Periodontology
Terapia parodontale: casi in aumento nei prossimi anni
in Pubblicazioni recentiIn base ad uno studio americano effettuato dalla Transparency Market Research, il mercato delle cure odontoiatriche è destinato a raddoppiare, toccando i 12 miliardi di dollari in USA. Un trend, questo, che interessa anche l’Italia, dove i casi di malattia paradontale sono in aumento.
Nell’articolo offerto da Odontoiatria33, troviamo il parere in merito del presidente SIdP Nicola Marco Sforza, che sottolinea la necessità delle campagne di prevenzione per evitare che la malattia si aggravi, nonché l’importanza della riduzione dell’invasività delle terapie, grazie alle nuove tecnologie e risorse attualmente disponibili.
Aladent contribuisce alla prevenzione e alla cura delle parodontoti. Inoltre risponde al requisito posto del presidente Nicola Marco Sforza di riduzione dell’invasività delle terapie.
Leggi l’articolo su Odontoiatria33.it
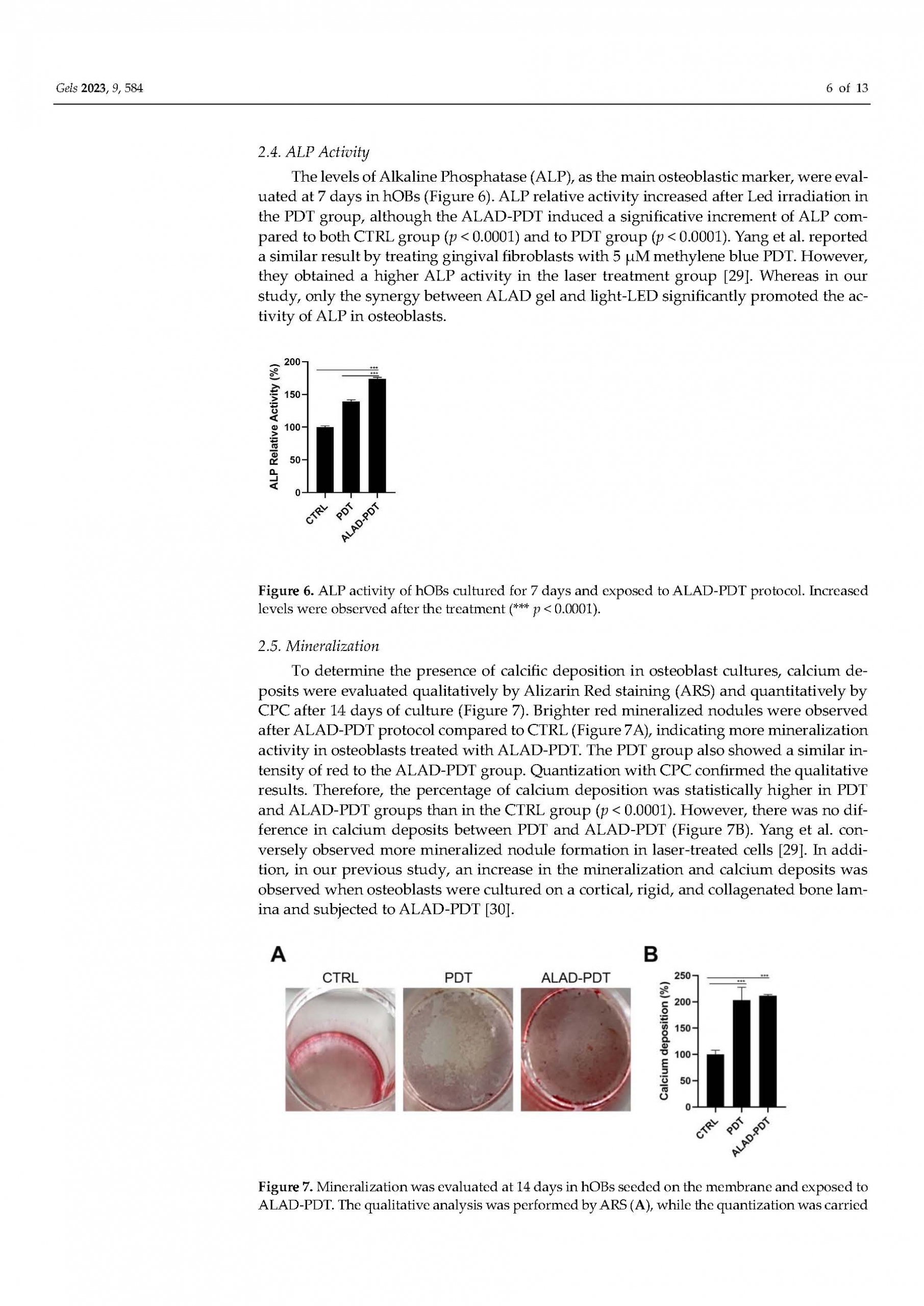
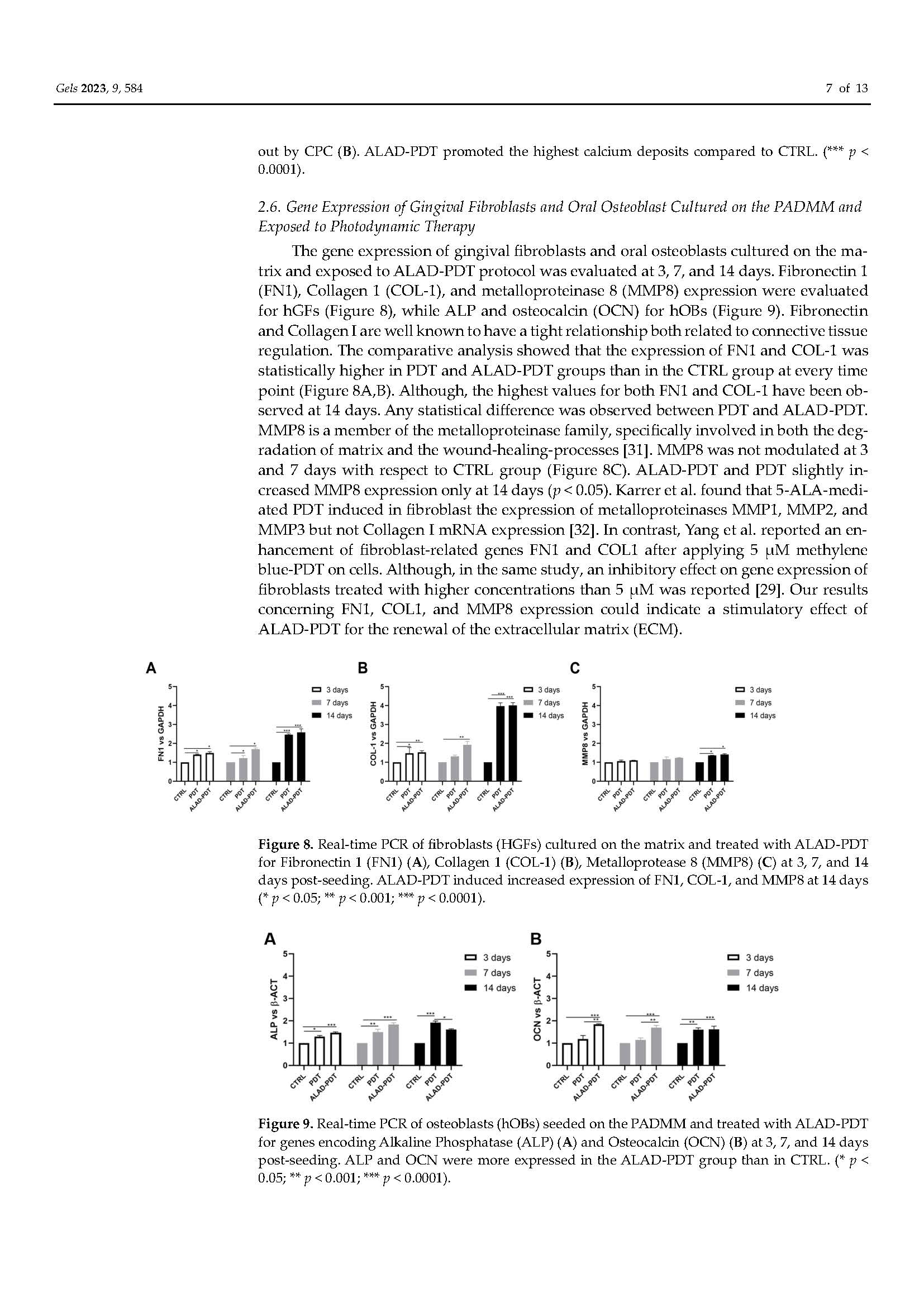
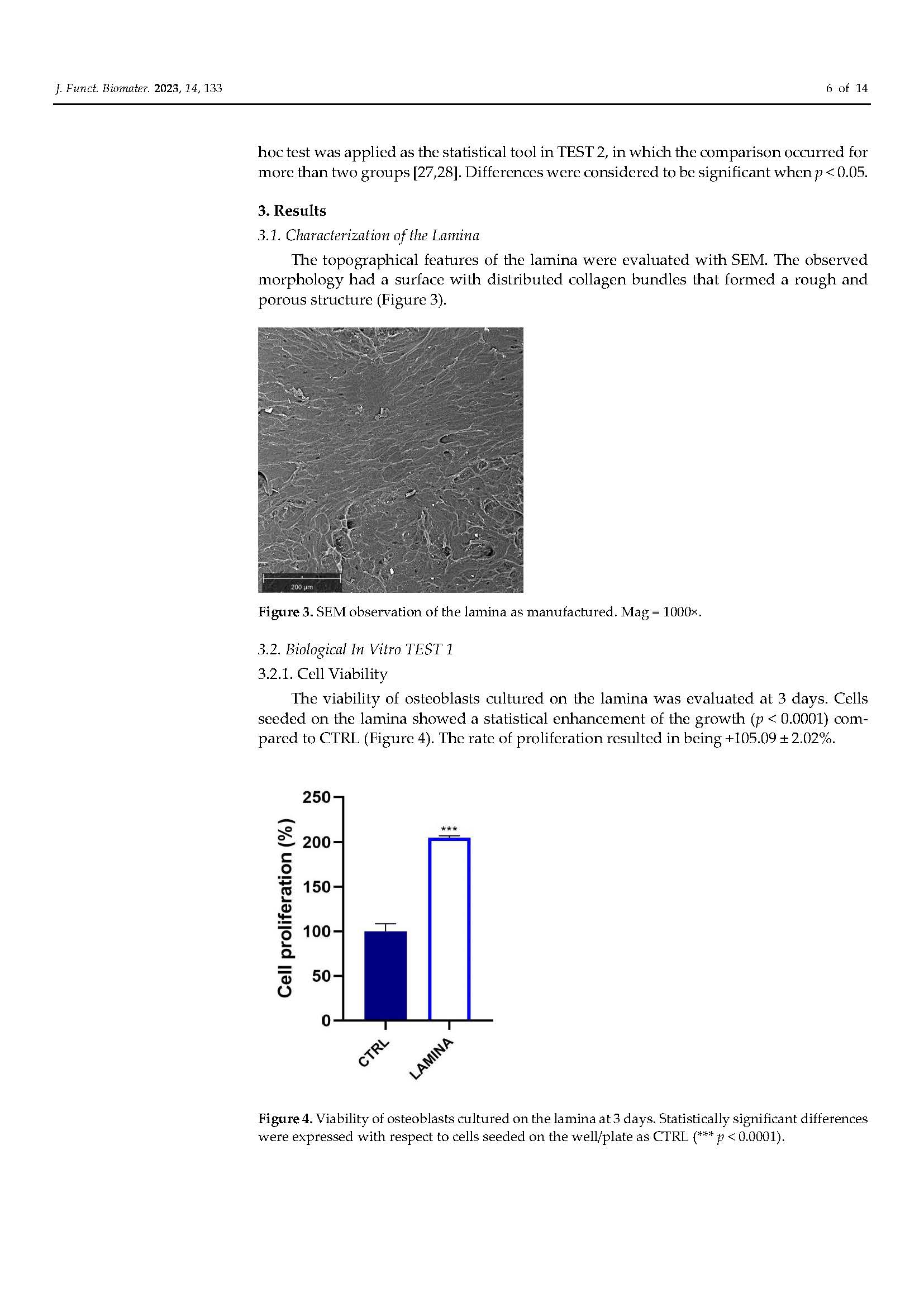
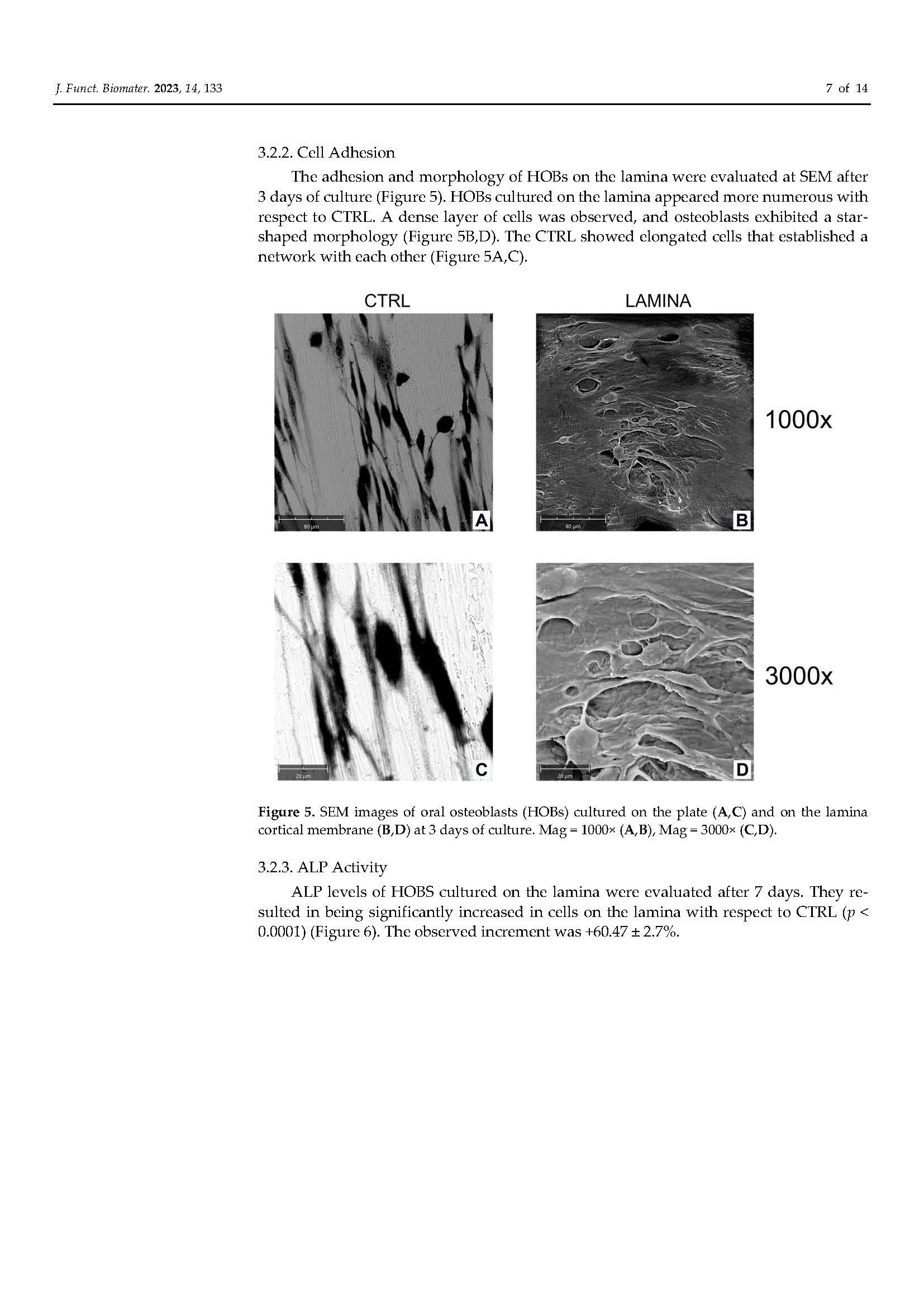
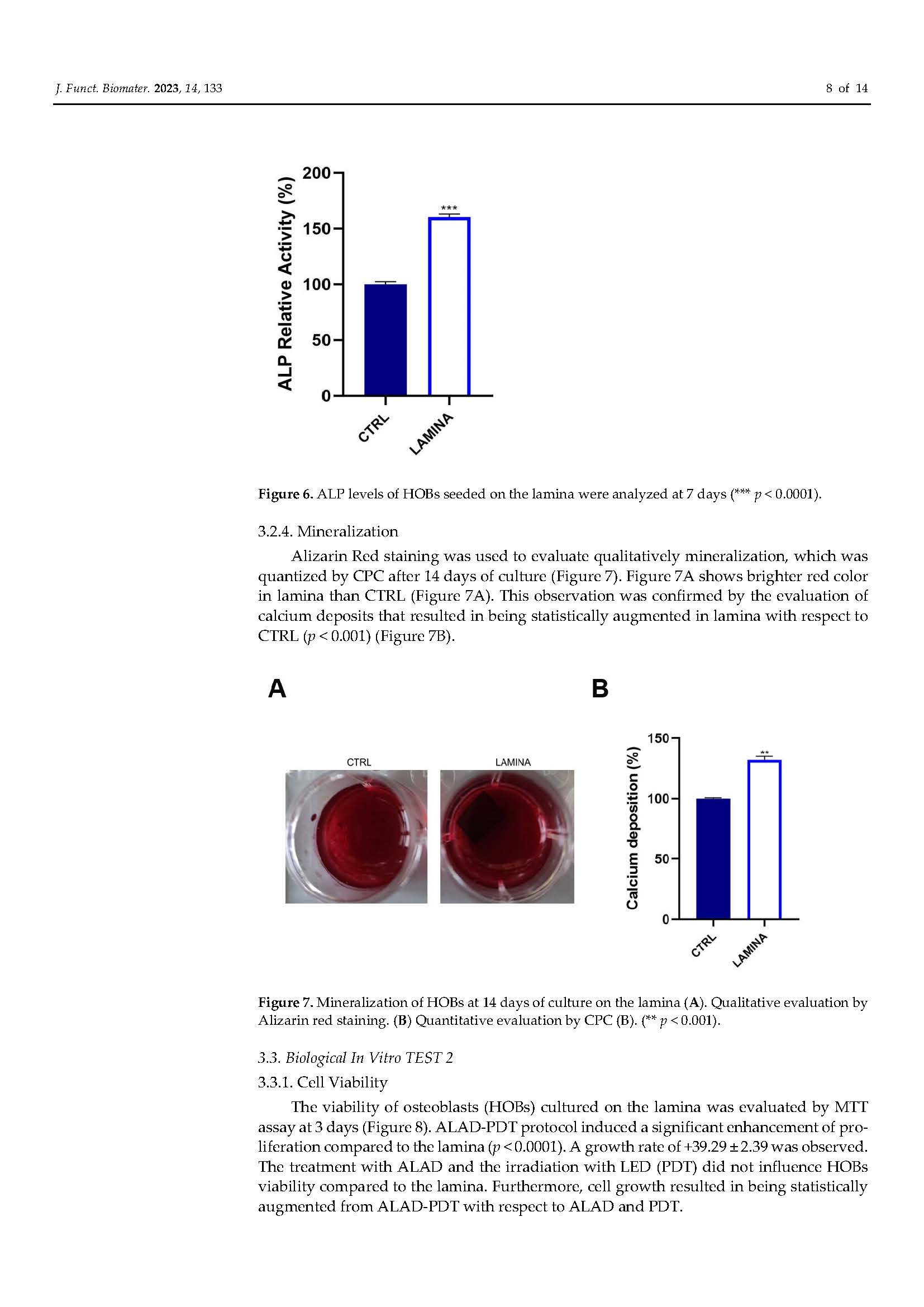
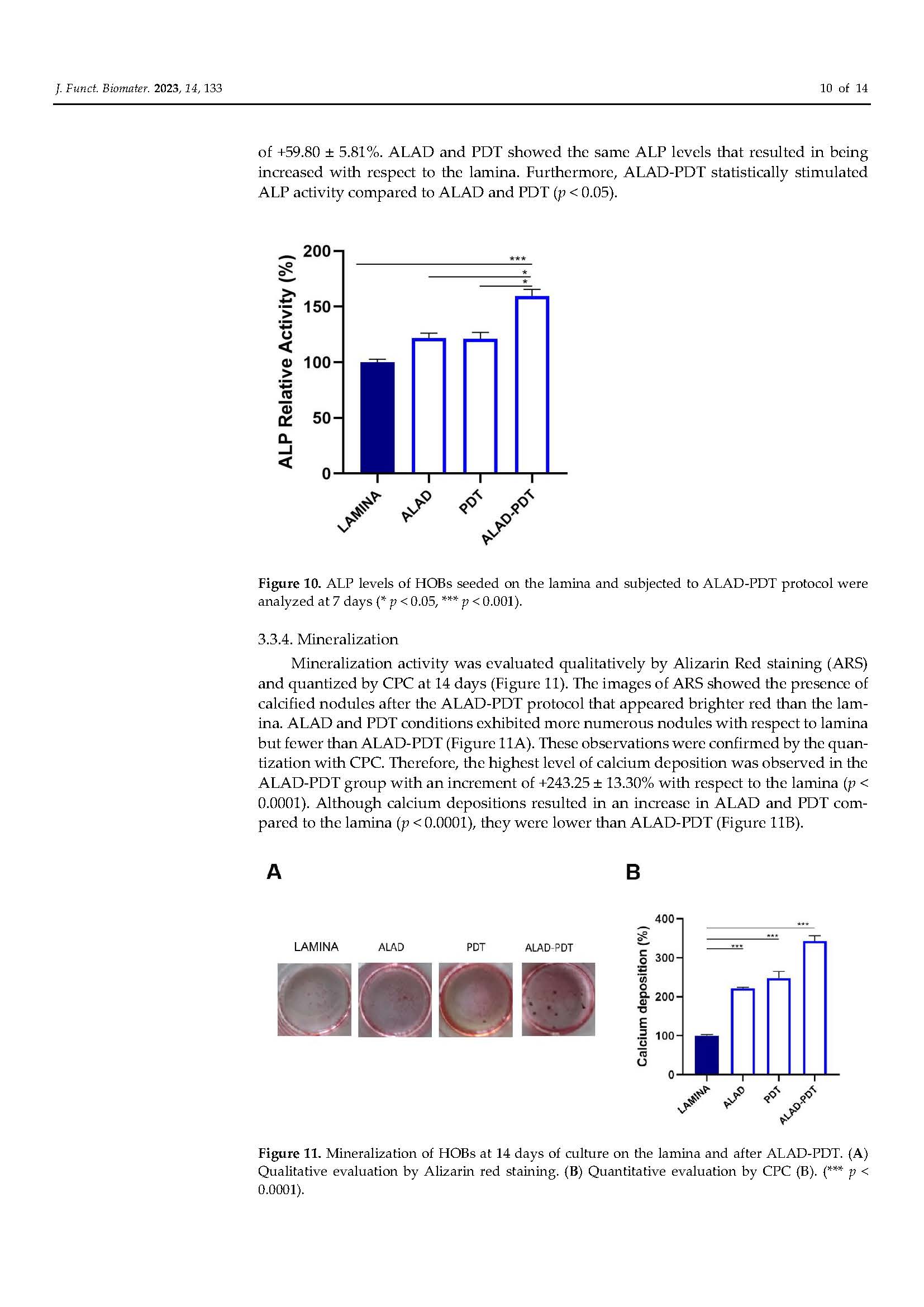
Functionalization of a Cortical Membrane with a Photodynamic Protocol
in Pubblicazioni recentiBONE RIGENERATION. The published article demonstrates that the adjunctive application of ALADENT -PDT to oral osteoblasts cultured on a cortical lamina provides an higher cellular proliferation and adhesion and increased matrix bone deposition. The level of calcium deposition was observed in the ALADENT-PDT group with an increment of +243.25 ± 13.30% versus the lamina alone.
Alphastrumenti Srl
Via Volontari del Sangue 4
20066 Melzo – MI
P.iva 06754120159
Email: info@aladent.it
Tel: +39.0295738540
Fax: +39.029551815